Debunking common myths about healthcare consumerism [INSIGHT]
December 8, 2015
Until recently, consumerism in the U.S. healthcare industry has moved slowly. However, several converging forces are likely to change the situation soon and result in a more dynamic market. Higher deductibles and copayments, greater transparency into provider performance and costs, and the rise of network narrowing and provider-led health plans are prodding patients to become more involved in healthcare decision making than ever before.
As yet, most payors and providers have comparatively little data to assess how consumerism is likely to affect them. As a consequence, they can neither confirm nor refute a number of assumptions about healthcare consumerism that are often stated as fact.
Over the past eight years, we have conducted extensive research into healthcare consumerism. This year alone, we surveyed more than 11,000 people across the country about how they perceive their healthcare needs and wants, how they select providers, and how they make other healthcare decisions. Our results suggest that many of the assumptions currently being made about healthcare consumerism are no more than myths.
Myth #1
Healthcare is different from other industries. Consumers don’t bring the same expectations about customer experience to healthcare that they bring to retail or technology companies.
Our findings indicate that consumers want the same qualities in healthcare companies that they value in non-healthcare settings. In this year’s Consumer Health Insights (CHI) survey, we asked participants to identify the non-healthcare companies with the strongest consumer focus. Apple and Amazon led the list. We then asked the participants to tell us what qualities gave such companies a strong customer focus, as well as what they valued in a consumer-focused healthcare company.
The answers to the two questions were surprisingly similar (Exhibit 1). For example, more than half the participants cited great customer service as important for nonhealthcare and healthcare companies alike. Other qualities that the participants identified as important for both sets of companies were delivering on expectations, making life easier, and offering great value.
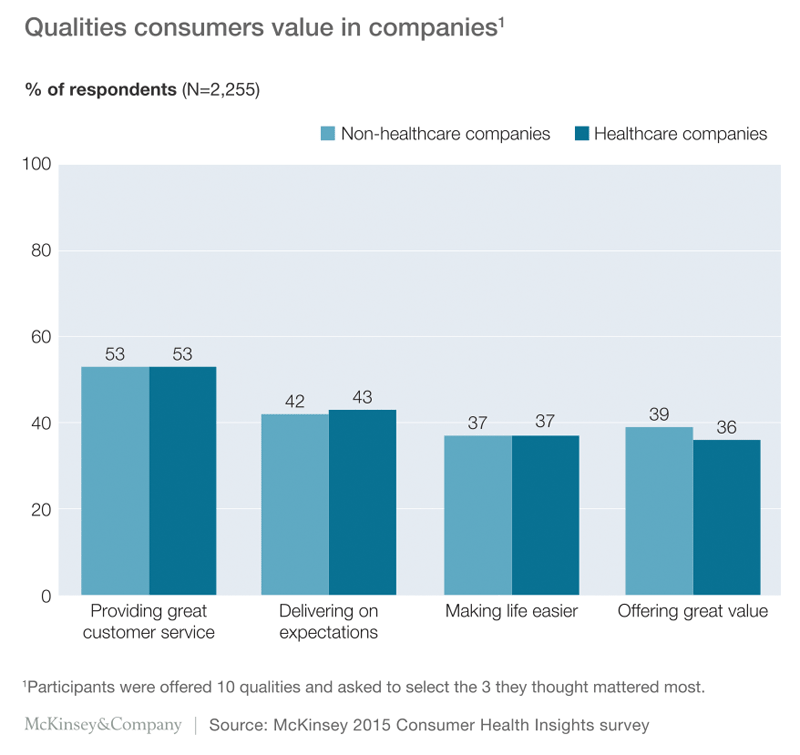
Whether healthcare companies need to perform as well as Apple and Amazon on customer experience remains to be seen. However, the evidence suggests that just performing better than other current healthcare competitors will not be sufficient. Customer expectations are being set by non-healthcare industries, and meeting those expectations is likely to be critical to ensure satisfaction and loyalty.
Myth #2
Consumers know what they want from healthcare companies and what drives their decisions.
Most consumers have strong opinions about what matters to them when they make healthcare decisions or receive healthcare services. The evidence suggests, however, that there is often a disconnect between what consumers believe matters most and what influences their opinions most strongly. Given the intangible nature of health insurance and healthcare provision, it appears that some factors play a much greater role than most consumers realize. For example, as part of our 2014 CHI survey, we posed two questions about patient satisfaction to the participants who reported having been hospitalized within the previous three years. First, we asked them how satisfied they were with their hospital experience. Second, we asked them to rank the importance of various factors that might have influenced their satisfaction levels.
More than 90% of these participants said they had been at least somewhat satisfied with the care they received, and most of them rated the outcome achieved as the most important influence on their satisfaction. However, when we mapped the factors that participants said influenced their satisfaction against their reported levels of satisfaction, we found that the empathy and support provided by health professionals (especially nurses) had a stronger impact than outcomes did (Exhibit 2). Satisfaction levels were also strongly influenced by the information the participants had been given during and after treatment.
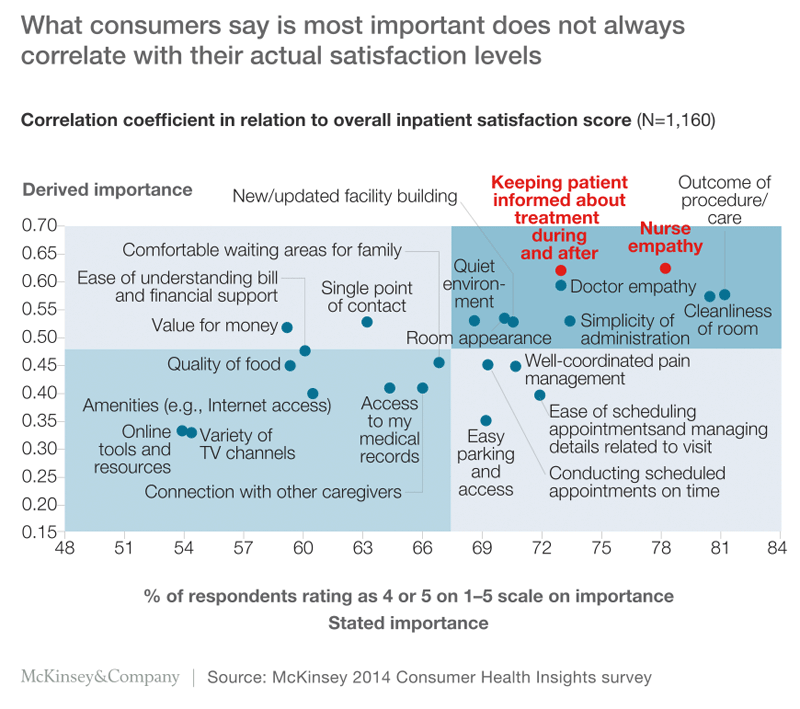
In general, our results suggest that people tend to overstate tangible factors (e.g., parking, pain management) and understate factors that are more emotional (e.g., empathy) or abstract (e.g., value).
Myth #3
Most consumers research their healthcare choices before making important decisions and then make fact-based choices based on their research.
Five different surveys we conducted recently suggest that many, if not most, healthcare consumers are not yet making research-based decisions. Our findings indicate, for example, that only a few consumers are currently researching provider costs or even the number of providers they can choose among. Although some (but far from most) consumers are beginning to research their health plan choices, many of them are not yet aware of key factors they should consider before selecting coverage.
Provider choices. In this year’s CHI survey, only 22% of the participants said that they always ask about cost before going to a doctor or other healthcare provider. We also asked participants whether they had received certain services in the past year and, if so, whether they had researched costs in advance. Exhibit 3 shows the results. The participants who received maternity care were most likely to report that they had researched costs prospectively. In all cases, the participants were much more likely to say that they had “talked to someone” (e.g., a provider or insurance representative) to investigate costs than to look at websites. Furthermore, even among the subset of consumers who reported doing research on costs before undergoing an expensive, invasive procedure (e.g., cardiac or joint surgery), half still said that their doctor’s recommendation was the key factor that influenced their decision about where to seek care.
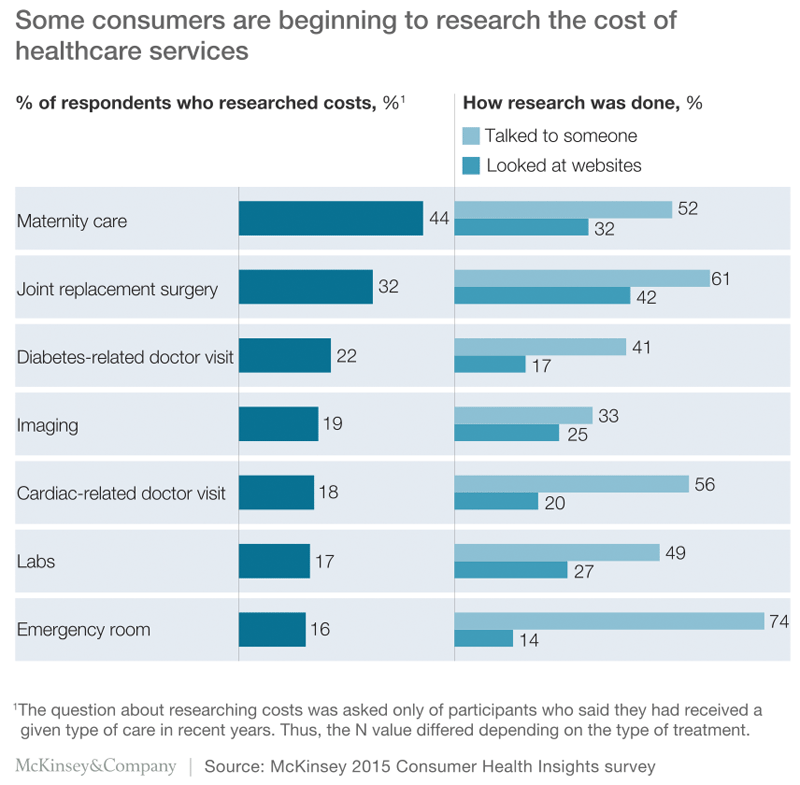
Cost is not the only factor most consumers are not yet actively investigating. In last year’s CHI survey, we asked the participants who reported having been hospitalized in the previous three years to tell us how many hospitals there were in their local area. More than half said there was only one local hospital when, in fact, there were a median of three hospitals within a 10-mile radius of their home and ten hospitals within a 20-mile radius.
Health plan choices. Soon after the close of the 2015 open enrollment period (OEP), we surveyed consumers who were eligible to purchase exchange plans to investigate the decisions they made about health insurance during the OEP.1 Forty-four percent of those who said they have bought an exchange plan for the first time indicated that they did not understand the type of provider network included in their plan. Nineteen percent of those who had purchased an exchange plan last year also indicated they were unaware of their plan’s provider network. Only 12% of those who remained uninsured knew the size of the subsidy they were eligible for, and only 59% were aware of the penalty for not obtaining coverage.
Similarly, in our survey this year of Medicare members, we found that only 21% of those who had enrolled in a Medicare Advantage (MA) plan knew their plan’s Star rating. However, almost all of those who knew their plan’s rating had purchased a plan that had three or more stars.
Moreover, in a survey we conducted this year of Medicaid-eligible recipients, only 32% of those who were enrolled in a managed care program and did not have dual Medicare coverage indicated that they had done any research before selecting a carrier, even though they had the option of choosing among multiple carriers.
Myth #4
Now that consumers are paying more for their healthcare, premium price is the only truly important factor in purchase decisions.
During both the 2014 and 2015 OEPs, premium price was, indeed, an important factor for many consumers. However, a sizeable percentage of people did not buy the cheapest plan available to them.
In our 2015 post-OEP survey, for example, 49% of the participants who had purchased exchange plans and remembered the plans’ pricing said that they had selected products with premiums that were average or above-average relative to the other plans within the comparable metal tier. The higher-premium products these participants bought (in comparison with the less-expensive plans purchased by other respondents) were more likely to be based on preferred provider organizations, to include pharmacy benefit add-ons, or to cover alternative types of care (e.g., acupuncture, chiropractic).
A subsequent report released by the Department of Health and Human Services confirms that price is not the only factor that many people shopping for individual coverage consider.2 It found that 66% of the 8.84 million people who bought health insurance through the federally facilitated marketplace during the 2015 OEP could have purchased a health plan with a monthly premium of $50 or less (after the advanced premium tax credit was applied). However, only about half of these people bought the very-low-cost plans.
In our Medicare study, we asked participants to design their own plan, giving them trade-offs between premium prices and various cost-sharing and benefit options (e.g., premiums went up as deductibles went down). Only 15% of the participants selected a $0 premium plan. In contrast, almost two-thirds of them said they would be willing to pay a $50 premium per month if it would reduce their medical deductible to $0. Thirty percent of the participants said that they would be willing to pay more than they were currently paying if it would help them hold their deductible down or enabled them to buy ancillary products. The feature cited most often by those willing to pay higher premiums was having a $0 deductible for prescription drugs.
Similarly, in this year’s CHI survey, one-third of the participants said they were willing or very willing to pay up to 20% more for health insurance if it gave them more choices about where to seek care. Furthermore, in a private exchange simulation we conducted recently with individuals covered by employer-sponsored insurance, the participants spent, on average, 40% above the employer contribution level to obtain ancillary benefits, such as vision, life, and critical illness insurance. In fact, many of the private exchange simulation participants were willing to trade down on medical benefits so they could trade up on ancillary benefits (Exhibit 4).
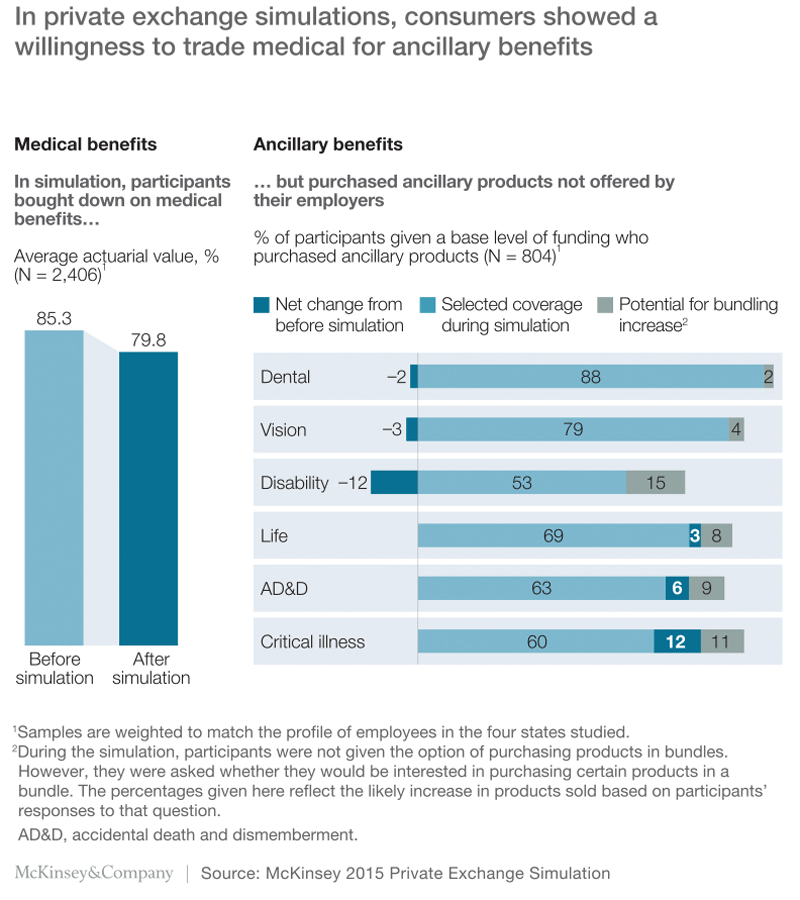
Myth #5
Almost all consumers have a primary care provider (PCP) and are highly reluctant to change doctors.
In this year’s CHI survey, 82% of participants said that they had a regular PCP. However, the likelihood of having a PCP was age-related: 96% of the participants above age 65 reported having a PCP, compared with only 65% of those ages 18 to 34. The likelihood of having a PCP was also influenced by income (89% of those with incomes above $100,000 said that they had a PCP) and health status (90% of those with one or more chronic conditions had a PCP).
Among all of the participants who did have a regular PCP, 66% said that they would not change providers unless they or their doctor moved. However, 57% of them also indicated that they would be willing to switch doctors if their health plan no longer covered their PCP. Among this 57%, willingness to switch was influenced by the length of a participant’s relationship with the PCP: 72% of those who had been using that doctor for only one or two years were willing to make the change, compared with 53% of those who had been with their doctor for five or more years.
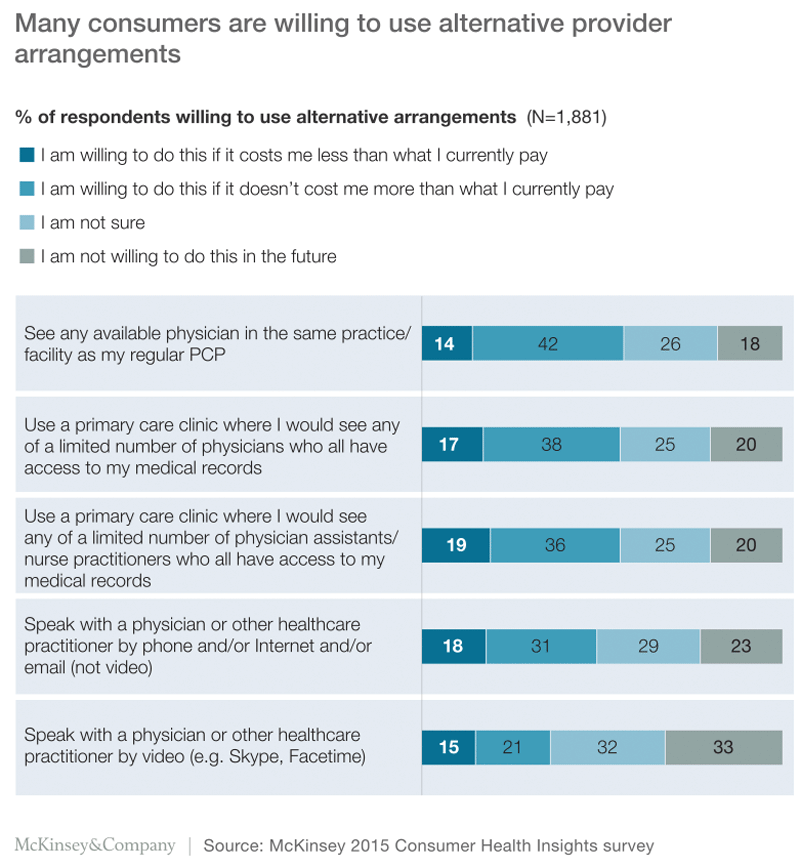
Other evidence from this year’s CHI suggests that many consumers are willing to consult providers other than a regular PCP. For example, 71% of all of the participants agreed with the statement: “There are many good primary care physicians that I would be satisfied seeing.” Forty-five percent of the participants said that they had made an appointment at least once with any available doctor within the same practice or facility as their regular PCP. Of those who had not done so, only 18% indicated that they were unwilling to consult any doctor but their PCP.
In addition, 16% of the participants said that they receive routine care from a multidoctor primary care clinic rather than an individual PCP. When asked why, nearly half of these participants cited accessibility (e.g., convenient locations, shorter waiting times, easier scheduling). Among the 84% of participants who did not receive care from a primary care clinic, 55% said they would be willing to do so if it cost no more than or less than what they currently pay (Exhibit 5).
Myth #6
Retail clinics will remain a niche health solution.
Awareness and utilization of other alternative-care options are also rising. In this year’s CHI survey, more than 80% of the participants were aware of healthcare services being offered through pharmacies and retail stores. About half of these participants, however, were unsure of the specific services being offered.
About two-thirds of the participants said they are willing to use healthcare services offered by a pharmacy or retail store. Twenty percent reported having already sought care in these settings within the past two years (up from 10% in our 2013 CHI survey). The chief reason given for using pharmacies and retail clinics for care was, once again, accessibility (convenient locations, not needing an appointment, convenient hours). More than three-quarters of the 2015 participants who had used these alternative-care options said they plan to do so again.
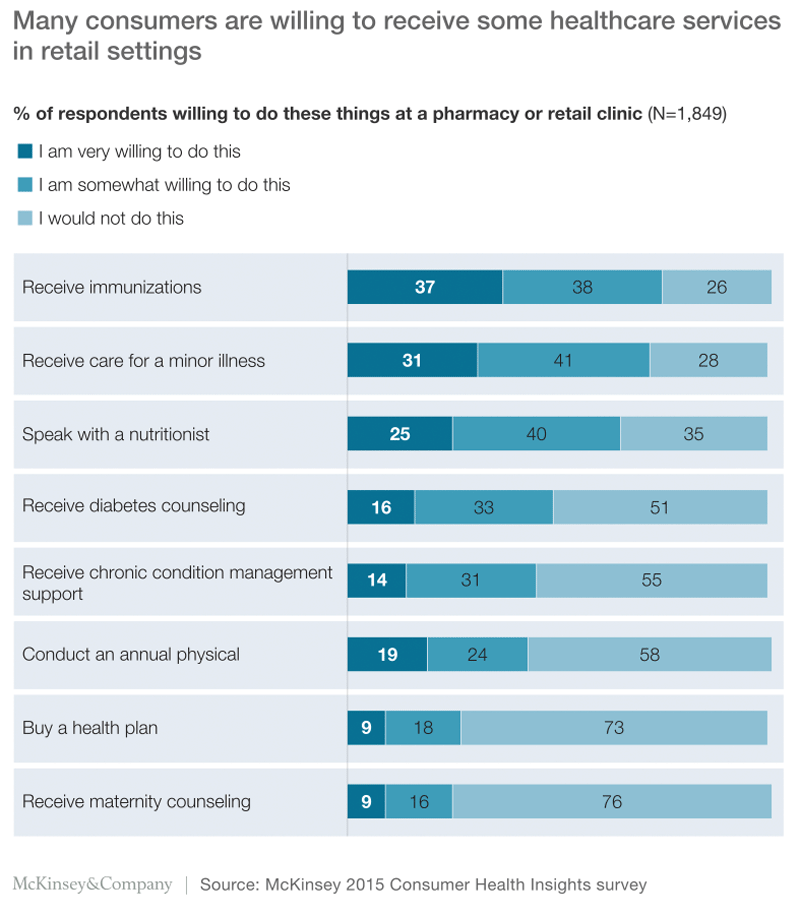
Just over half (51%) of those who reported having received healthcare services at a pharmacy or retail clinic indicated that they had done so for immunizations; 26% said they had sought treatment for a minor illness. Of the participants who said they had not yet used one of these alternative-care options, more than 60% indicated they were willing to do so for immunizations, minor illnesses, or nutritional/weight loss support (Exhibit 6).
Use of these alternative care options could grow substantially in the next few years, given their increasing numbers and expanding offerings. The number of retail clinic locations across the United States rose from 1,183 in 2010 to 1,866 in 2015.3 CVS, which operates about half of the retail clinics, has announced that it plans to have 1,500 clinics by 2017. Growth among other the major players is likely to accelerate now that Walmart is putting primary care practices within its stores, and Walgreens is partnering with Theranos to offer convenient, affordable blood testing.
Myth #7
Only young people are using technology to manage their health and healthcare needs.
In both this year’s and last year’s CHI surveys, we also asked participants about using technology to manage their health and healthcare needs. Not surprisingly, millennials (those between the ages of 18 and 34) were more likely to report using technology for these purposes, but a considerable number of the older participants were doing so as well (Exhibit 7). In all age groups, the top two activities were communicating with doctors and scheduling appointments. However, millennials were much more likely than older participants were to say that they were using social media to share wellness ideas and participate in online wellness groups.
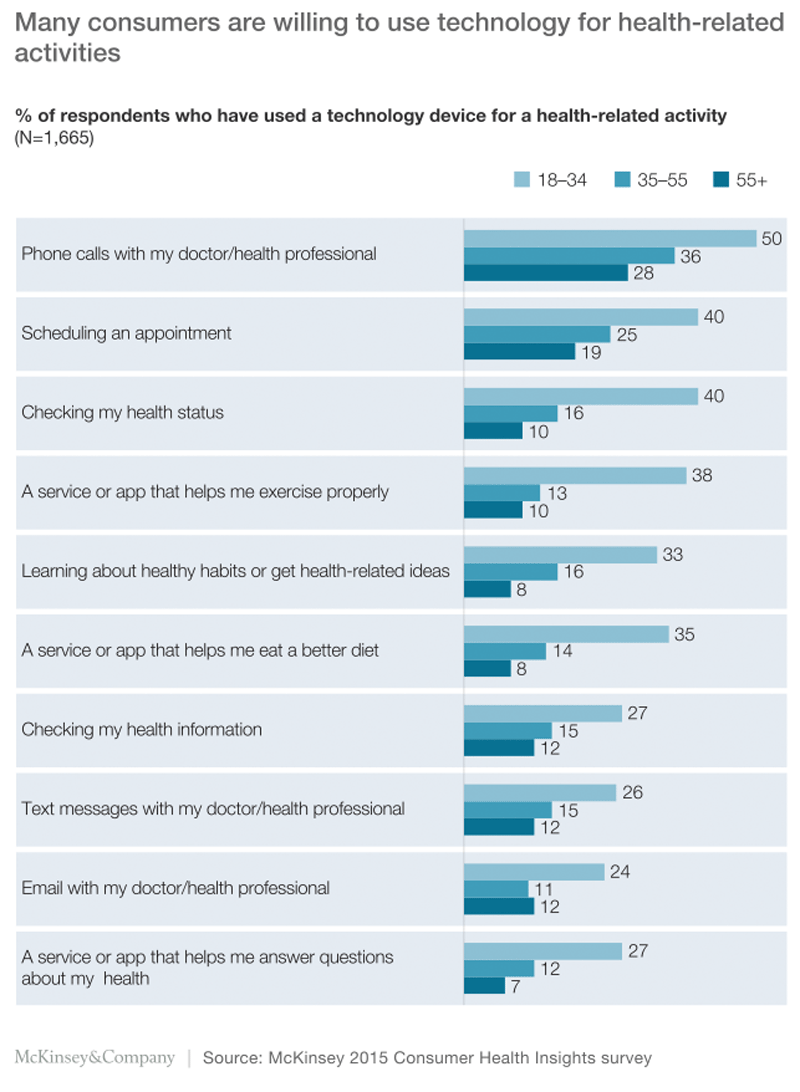
We also asked participants about whether they had used website or apps for a number of health-related activities, and, if so, whether they thought those resources were more or less effective than phone or in-person communication. For two of the most common activities—communicating with a physician and scheduling appointments—the majority of participants age 65 and older (65% and 78%, respectively) thought that websites and apps were more effective.
Myth #8
Most people are willing to trust insurers to store their health records.
In our 2014 CHI survey, we asked the participants to imagine having some sort of health monitoring device. We then asked them two questions: Where would they be comfortable storing information from that device? And with whom would they be willing to share the data?
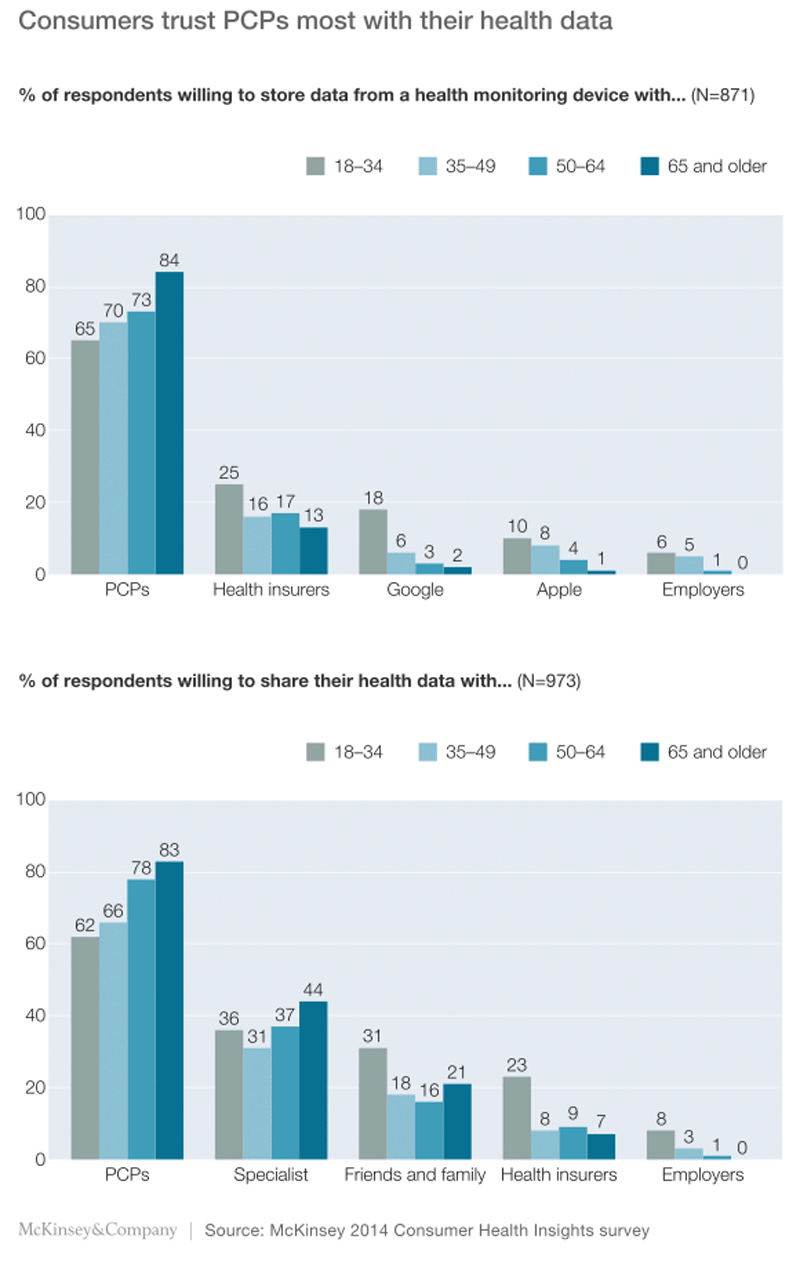
Apropos storage, the participants overwhelmingly chose PCPs (Exhibit 8). Only a minority of them said they were comfortable having health insurers, Google, or Apple store their health data, and even fewer people chose employers. Participants also named PCPs as the group with whom they were most comfortable sharing the data (Exhibit 8). In both cases, age had only a small impact on the answers received.
We believe that healthcare consumerism will soon enter the steep slope of the innovation S curve and become a much more significant force. Payors and providers need to begin making plans now if they want to be ready to respond to, and perhaps shape the evolution of, healthcare consumerism.
The data and insights we have amassed can help them do that. Our findings suggest, for example, that payors should think about what value proposition they want to offer to consumers. That value proposition can be, but doesn’t have to be, price related—consumers are open to other enticements. And payors should not assume they are the natural owners of consumers’ health records; they will have to find a way to earn greater consumer trust if they want to do that. Providers should not take patient loyalty for granted or underestimate the role that experience-related factors such as convenience and empathy play in consumer satisfaction and loyalty.
The results described in this article are only a fraction of the information we have amassed. Our findings also reveal important attitudinal differences based on age, gender, ethnicity, income, health status, and geography—differences that have important implications for both payors and providers. These findings have convinced us that both payors and providers need to better understand what really drives consumer decision making and focus on that (rather than just on what consumers say). This understanding must be based on very granular data to ensure its relevance to local healthcare players.
In addition, both payors and providers should think about the evolving role of new healthcare technologies in shaping consumer behaviors so they can take advantage—and not become victims—of them. Perhaps most important, both payors and providers should realize that consumers’ expectations are no different in healthcare than in any other industry. In fact, other industries will continue to shape these expectations—healthcare companies need to catch up, or they risk being disrupted.
About the authors
Jenny Cordina is a principal in McKinsey’s Detroit office, Rohit Kumar is an associate principal in the Chicago office, and Christa Moss is a consultant in the Cleveland office.
The authors would like to thank Erica Coe, Elizabeth Jones, Katherine Linzer, Elina Onitskansky, Kyle Weber, and Emir Roach for their contributions to this article.





























